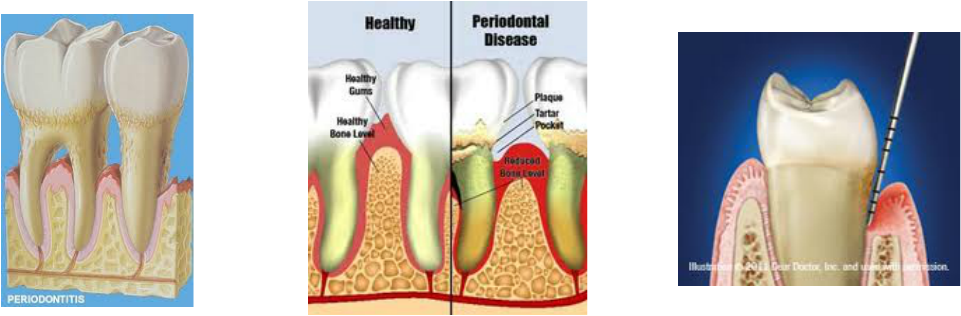
Periodontitis
Review of Journal Article
The journal article i chose is called, "Genetic and Environmental Risk Factors for Chronic Periodontitis".
Periodontitis is a bacterial infection of the periodontium. The periodontium is the supporting tissues of the teeth. This results in destruction of all four parts of the periodontium including the gums, the periodontal ligament, the bone, and the cementum. Results of this destruction is irreversible to the tissues of the periodontium. The most common form of periodontitis is chronic periodontitis. It is most commonly seen in adults over 35 years of age. It is initiated by the dental plaque biofilm. The distinguishing diagnostic factors include the following; irreversible loss of attachment and bone loss, swelling, redness, gingival bleeding, periodontal pockets, tooth mobility, pus, bad taste in mouth, sensitive teeth, and spaces in between teeth. With chronic periodontitis the destruction present is consistent with the amount of dental plaque. The etiology of periodontitis can be systemically related or it can be caused by local factors. Some systemic factors associated with periodontitis includes; Cardiovascular disease, Pregnancy, Diabetes, Osteoporosis, AIDS, leukemia, down syndrome, hormonal variations, medications and Respiratory disease. Some local risk factors contributing to periodontitis includes; faulty restorations, inadequate professional and self-care, stress, poor dieting, dental calculus, traumatic factors and smoking. The pathogens associated with periodontitis include; Aggregatibacter Actinomycetemcomitans, Tannerella Forsythia, and Porphyromonas Gingivalis. The AAP classification of chronic periodontitis is type II. The prevalence of chronic periodontitis is about 18% in the age group of 35 years or older. Some factors to include when educating your patients would be Oral Hygiene Instructions, showing them
how to floss correctly and how they should be brushing their teeth to be most
effective for that individual, and smoking cessation counseling if needed. Also letting them know if they have any systemic diseases, they would want to make sure they are under control so their periodontitis is lessened. The treatment recommendations would be to control the bacteria, by doing periodontal instrumentation, eliminate any risk factors, arrest disease progression, and to prevent the recurrence of the disease, by doing meticulous oral hygiene, by brushing, and flossing. The maintenance recommendations would be adequate self-care, coming to their recall intervals when recommended, usually a 3-4 month interval, and of course brushing twice a day, flossing once a day, they also can use a tongue scrapper and mouth wash. Another maintenance recommendation would be to
maintain a well balanced healthy diet.
Periodontitis is a bacterial infection of the periodontium. The periodontium is the supporting tissues of the teeth. This results in destruction of all four parts of the periodontium including the gums, the periodontal ligament, the bone, and the cementum. Results of this destruction is irreversible to the tissues of the periodontium. The most common form of periodontitis is chronic periodontitis. It is most commonly seen in adults over 35 years of age. It is initiated by the dental plaque biofilm. The distinguishing diagnostic factors include the following; irreversible loss of attachment and bone loss, swelling, redness, gingival bleeding, periodontal pockets, tooth mobility, pus, bad taste in mouth, sensitive teeth, and spaces in between teeth. With chronic periodontitis the destruction present is consistent with the amount of dental plaque. The etiology of periodontitis can be systemically related or it can be caused by local factors. Some systemic factors associated with periodontitis includes; Cardiovascular disease, Pregnancy, Diabetes, Osteoporosis, AIDS, leukemia, down syndrome, hormonal variations, medications and Respiratory disease. Some local risk factors contributing to periodontitis includes; faulty restorations, inadequate professional and self-care, stress, poor dieting, dental calculus, traumatic factors and smoking. The pathogens associated with periodontitis include; Aggregatibacter Actinomycetemcomitans, Tannerella Forsythia, and Porphyromonas Gingivalis. The AAP classification of chronic periodontitis is type II. The prevalence of chronic periodontitis is about 18% in the age group of 35 years or older. Some factors to include when educating your patients would be Oral Hygiene Instructions, showing them
how to floss correctly and how they should be brushing their teeth to be most
effective for that individual, and smoking cessation counseling if needed. Also letting them know if they have any systemic diseases, they would want to make sure they are under control so their periodontitis is lessened. The treatment recommendations would be to control the bacteria, by doing periodontal instrumentation, eliminate any risk factors, arrest disease progression, and to prevent the recurrence of the disease, by doing meticulous oral hygiene, by brushing, and flossing. The maintenance recommendations would be adequate self-care, coming to their recall intervals when recommended, usually a 3-4 month interval, and of course brushing twice a day, flossing once a day, they also can use a tongue scrapper and mouth wash. Another maintenance recommendation would be to
maintain a well balanced healthy diet.
References:
Nield-Gehrig, Jill, & Willmann, D.E. (2011). Foundation of Periodontics for
The Dental Hygienist. Third Edition.
Stabholz, A., Soskolne, W., & Shapira, L. (2010). Genetic and environmental risk factors for chronic periodontitis and aggressive periodontitis. Periodontology 2000, 53138-153. doi:10.1111/j.1600-0757.2010.00340.x
Nield-Gehrig, Jill, & Willmann, D.E. (2011). Foundation of Periodontics for
The Dental Hygienist. Third Edition.
Stabholz, A., Soskolne, W., & Shapira, L. (2010). Genetic and environmental risk factors for chronic periodontitis and aggressive periodontitis. Periodontology 2000, 53138-153. doi:10.1111/j.1600-0757.2010.00340.x